
The dual challenge of managing Autism Spectrum Disorder (ASD) and Epilepsy is a reality for many families.
These conditions often travel together, sharing underlying biological pathways.
As traditional medical interventions sometimes reach a plateau, the focus of regenerative medicine has shifted toward stem cells.
These biological building blocks offer a multifaceted approach that addresses the core neurodevelopmental and neurological issues present in both conditions.
It is estimated that nearly one-third of individuals diagnosed with Autism also experience seizures.
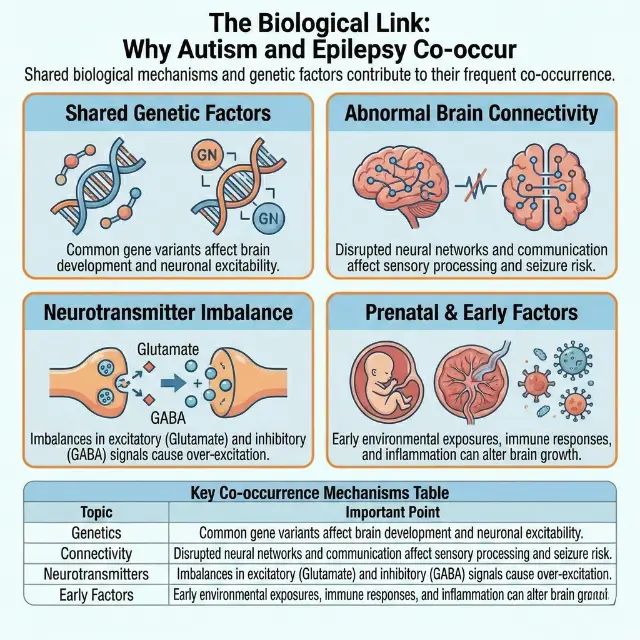
This is not a coincidence. Researchers have identified that both conditions often stem from:
Because stem cells—specifically Mesenchymal Stem Cells (MSCs)—possess powerful anti-inflammatory and regenerative properties, they are uniquely positioned to address these shared roots.
By targeting the "environment" of the brain, stem cells help recalibrate the neurological system, providing relief for both behavioral symptoms and seizure activity.
When we discuss stem cells, we are talking about a "smart" therapy. Unlike static medication, stem cells respond to signals of damage or inflammation.
Here is a breakdown of their primary functions in neurological repair:
Families researching these therapies often look for hard data. Recent clinical observations have shown significant shifts in quality-of-life scores following the administration of stem cells.
The following table summarizes the typical improvements reported in patient cohorts undergoing stem cell therapy for the dual diagnosis of ASD and Epilepsy:
| Improvement Category | Impact on Autism Symptoms | Impact on Epilepsy Symptoms |
| Communication | Enhanced verbalization and eye contact | Better post-seizure recovery (shorter "fog") |
| Behavioral Stability | Reduction in self-injury and hyperactivity | Lower frequency of irritability-linked seizures |
| Seizure Frequency | Potential reduction in "trigger" sensitivity | Up to 40-60% reduction in seizure episodes |
| Cognitive Function | Better focus and learning retention | Improved mental clarity and processing speed |
| Social Integration | Increased interest in peer interaction | Higher confidence due to stabilized health |
For children and adults on the spectrum, the goal is often independence and better social integration. The application of stem cells targets the "noise" in the brain.
When neuroinflammation is reduced, the individual can process sensory information more effectively.
In epilepsy, the primary concern is the uncontrolled electrical discharge in the brain.
Traditional anti-epileptic drugs (AEDs) focus on suppressing these discharges, but they don't "heal" the underlying tissue. Stem cells offer a different path.
Not all stem cells are the same. In the context of neurological disorders, the source and type of the stem cells matter significantly for safety and efficacy.
| Stem Cell Type | Source | Primary Advantage | Safety Profile |
| Umbilical Cord MSCs | Cord Tissue (Post-birth) | Highest potency and rapid replication | High (Non-invasive, no rejection) |
| Adipose MSCs | Patient's own fat tissue | Easy to harvest in large quantities | Moderate (Requires minor liposuction) |
| Bone Marrow MSCs | Patient's bone marrow | Long history of clinical use | Moderate (Requires painful extraction) |
| Neural Stem Cells | Specialized lab cultures | Highly targeted to brain tissue | Emerging (Under intensive research) |
When exploring stem cell therapy, the process is designed to be as minimally invasive as possible.
Most protocols involve an intravenous (IV) infusion or an intrathecal administration (delivering the stem cells into the spinal fluid) to ensure they reach the central nervous system effectively.
While the term "cure" is avoided in chronic neurological conditions, stem cells are considered a transformative management tool. They aim to significantly reduce the severity of symptoms and improve daily functioning.
Every brain is unique. Some families report "awakening" or improved eye contact within weeks of the first stem cell application. However, the structural and anti-inflammatory changes typically peak between 3 and 9 months post-therapy.
When using Mesenchymal Stem Cells (especially from umbilical cord tissue), the risk of rejection is nearly zero because these cells are "immuno-privileged." This means the body does not recognize them as foreign invaders.
The convergence of Autism and Epilepsy creates a complex landscape for families to navigate. However, the "dual benefit" of stem cells provides a logical, science-backed strategy.
By addressing the fundamental cellular malfunctions—inflammation and oxidative stress—stem cells do more than just mask symptoms; they work toward a more balanced and healthy brain environment.
As research continues to evolve, the hope is that stem cell therapy will become a standard cornerstone of neurodevelopmental care, opening doors that were previously thought to be locked.
