
The journey to parenthood is a profound experience, yet for millions of families across the globe, it is a path marked by unexpected hurdles.
Infertility, once a diagnosis that left many with limited options, is now being challenged by the rapid advancements in regenerative medicine.
At the forefront of this revolution is stem cell therapy, a groundbreaking approach that offers more than just a temporary fix—it offers a biological reset.
For those who have exhausted conventional treatments like IVF or hormone therapies, stem cell therapy is emerging as a beacon of hope.
By utilizing the body’s own regenerative power, this science aims to repair damaged tissues and restore reproductive functions that were once thought to be permanently lost.
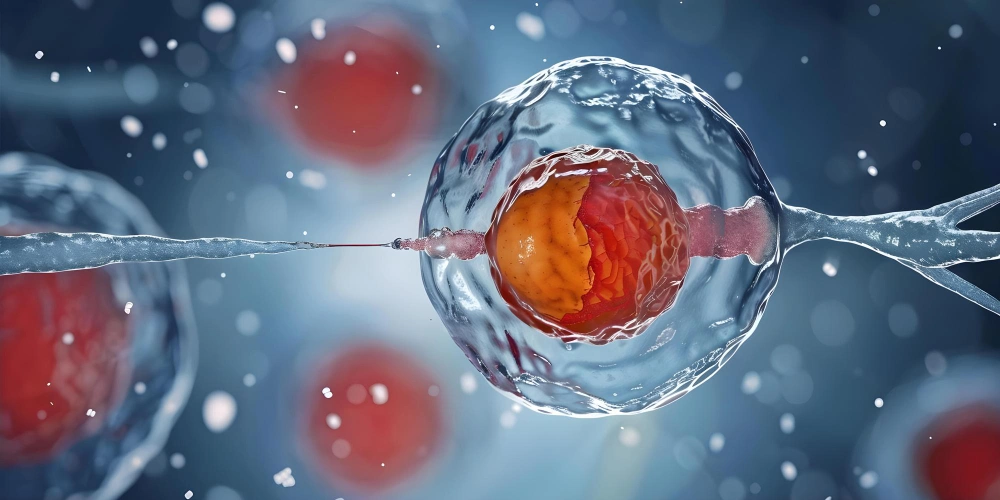
At its core, stem cell therapy relies on the unique ability of undifferentiated cells to transform into specialized cell types.
In the context of reproductive health, Mesenchymal Stem Cells (MSCs) are the "stars" of the show. These cells possess a remarkable "homing" instinct, allowing them to migrate to areas of inflammation or tissue damage within the reproductive system.
When a patient undergoes stem cell therapy, these cells work through paracrine signaling.
They release growth factors and anti-inflammatory cytokines that stimulate the repair of the ovarian environment or the testicular lining.
This isn't just about adding new cells; it’s about "waking up" the body's dormant biological processes.
For women, infertility often stems from issues related to egg quality, ovarian reserve, or the health of the uterine lining.
Stem cell therapy is currently being applied to several high-impact areas:
Premature Ovarian Insufficiency (POI) and Diminished Ovarian Reserve (DOR) are two of the most challenging diagnoses.
Recent clinical observations have shown that stem cell therapy can help "rejuvenate" the ovaries by promoting the development of healthy follicles.
By improving the microenvironment of the ovary, stem cell therapy helps increase the levels of Anti-Müllerian Hormone (AMH), a critical marker of fertility.
A thin or damaged uterine lining (often due to Asherman’s Syndrome) can prevent successful embryo implantation.
Stem cell therapy has shown incredible promise in increasing endometrial thickness.
By regenerating the lining, the uterus becomes more receptive, significantly boosting the success rates of both natural conception and assisted reproductive technologies.
To understand why so many families are turning to this science, we must look at the data.
Recent studies conducted through 2025 and early 2026 have provided compelling evidence of its efficacy.
| Condition Targeted | Success/Improvement Metric | Average Result Post-Therapy |
| Premature Ovarian Insufficiency | Oocyte Activation Rate | 70% |
| Thin Endometrium | Increase in Lining Thickness | 45% - 52% |
| Male Azoospermia | Sperm Detection in Ejaculate | 30% (Initial trials) |
| Diminished Ovarian Reserve | AMH Level Increase | 0.5 - 1.2 ng/mL improvement |
| Clinical Pregnancy Rate | Post-MSC Endometrial Repair | 25% - 28% |
For couples undergoing IVF, stem cell therapy may improve outcomes by:
Families who combine IVF with stem cell support often report higher chances of success and improved overall health.
Families searching for solutions in major Western medical hubs are increasingly looking for "natural" and "autologous" options.
This means using the patient’s own cells to avoid the risks of immune rejection.
If you are considering stem cell therapy, the process is designed to be streamlined and patient-centric.
One of the most frequent questions patients ask is: "How will I know if it worked?"
Clinical progress is usually monitored through specific biomarkers.
After undergoing stem cell therapy, patients often see a stabilization of the following:
Turkey has become a trusted destination for regenerative medicine and fertility care thanks to:
As we move further into 2026, the integration of stem cell therapy into mainstream fertility clinics is accelerating.
We are witnessing a shift from "managing" infertility to "curing" the underlying biological damage.
For families who have felt the heartbreak of failed IVF cycles, the regenerative potential of stem cell therapy offers a new timeline—one where biological parenthood is within reach.
Infertility is a complex challenge, but you do not have to face it with yesterday's tools.
Stem cell therapy represents the absolute frontier of what is possible in modern medicine.
By restoring function, improving hormone levels, and regenerating tissue, this therapy is rebuilding the foundation of the family.
If you are looking for a path that aligns with your body’s natural healing processes, stem cell therapy may be the answer you’ve been searching for.
The science is here, the results are grounded in data, and for many families, the hope is finally real.
