


The 21st-century landscape of medicine is undergoing a profound transformation. We are shifting away from traditional, mass-produced pharmaceutical interventions toward highly personalized biological therapies. At the forefront of this revolution is autologous stem cell therapy, which utilizes an individual's own biological resources to combat disease, repair tissue, and restore physiological balance. This blog explores the science behind autologous therapy, focusing on its biological mechanisms, safety advantages, clinical applications, and how organizations like Rumi Pulse are applying these innovations to complex conditions such as Autism Spectrum Disorder (ASD).
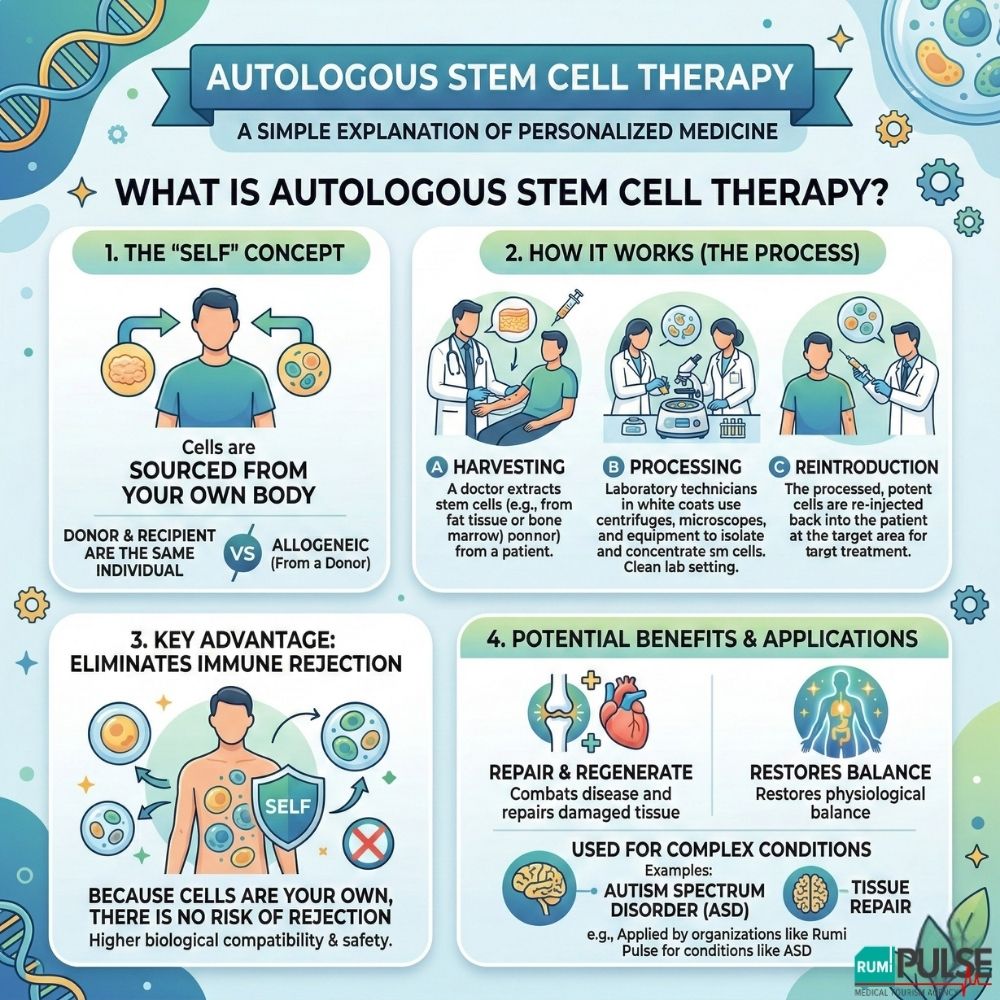
The term autologous comes from the Greek words "autos" (self) and "logos" (relation or logic). In a medical context, it refers to procedures where the donor and the recipient are the same individual. This is a key distinction from allogeneic therapies, where cells are sourced from a donor. By using the patient’s own cells, autologous therapy eliminates the risk of immune rejection, making it a safer and more biologically compatible treatment.
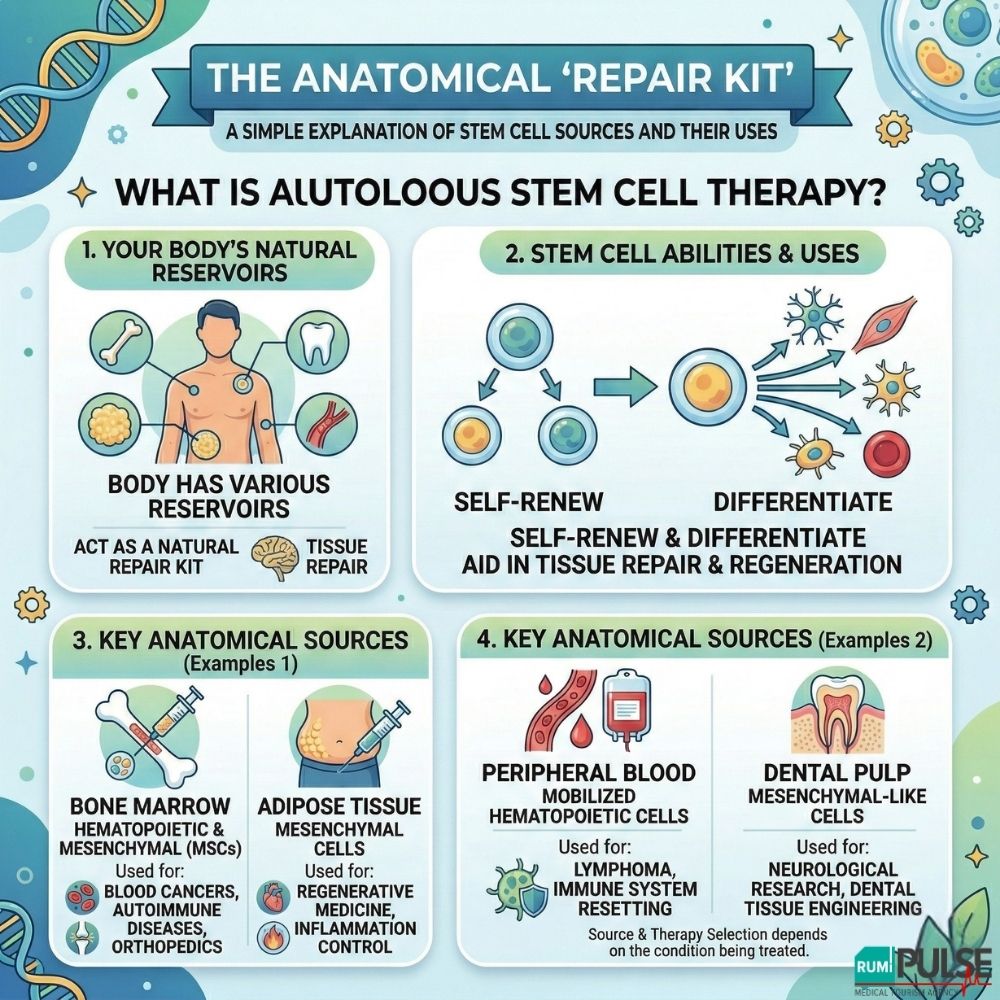
The human body maintains various reservoirs of stem cells throughout adulthood, which act as a natural "repair kit." These stem cells have the ability to self-renew and differentiate into multiple cell types, aiding in tissue repair and regeneration. The success of autologous stem cell therapy depends largely on the source of these cells, which include:
Each anatomical source offers unique therapeutic potential, with the selection largely depending on the condition being treated.
Autologous stem cell therapy is a sophisticated multi-step biological process. Research indicates that the therapeutic effect results from four primary mechanisms:
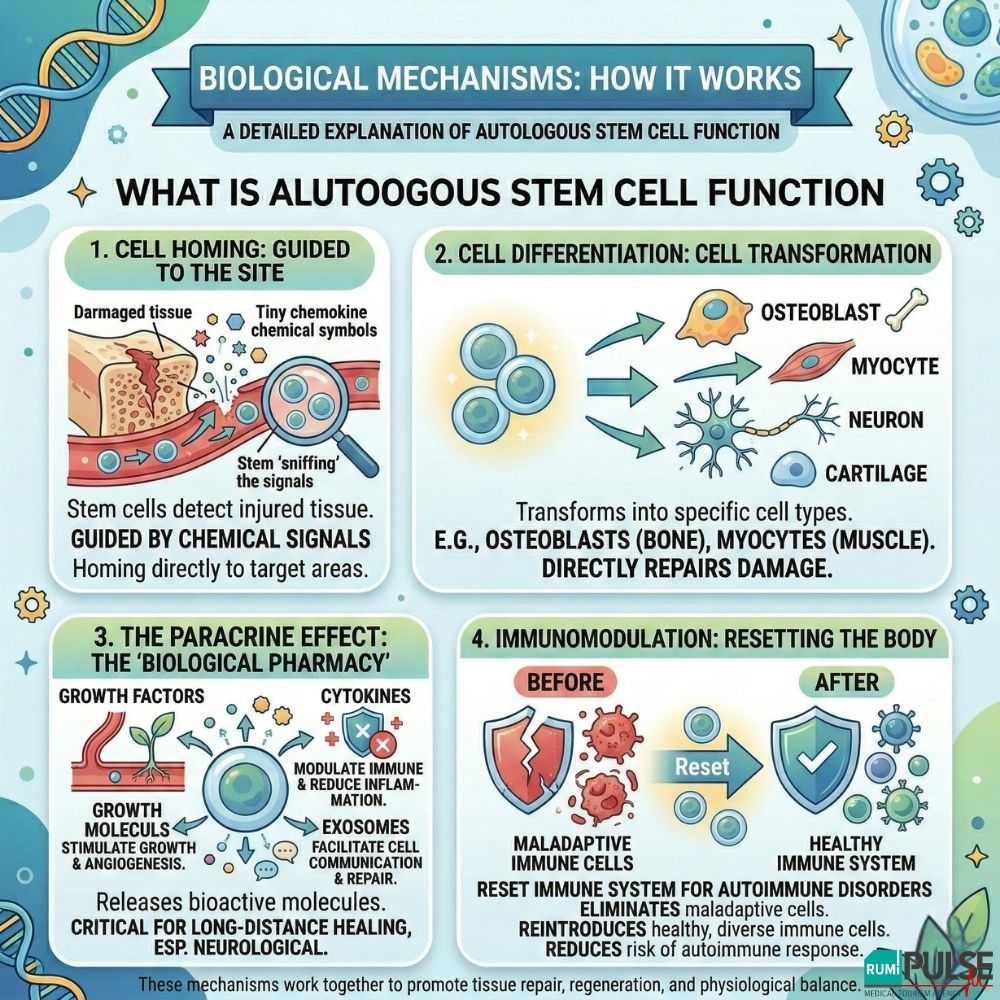
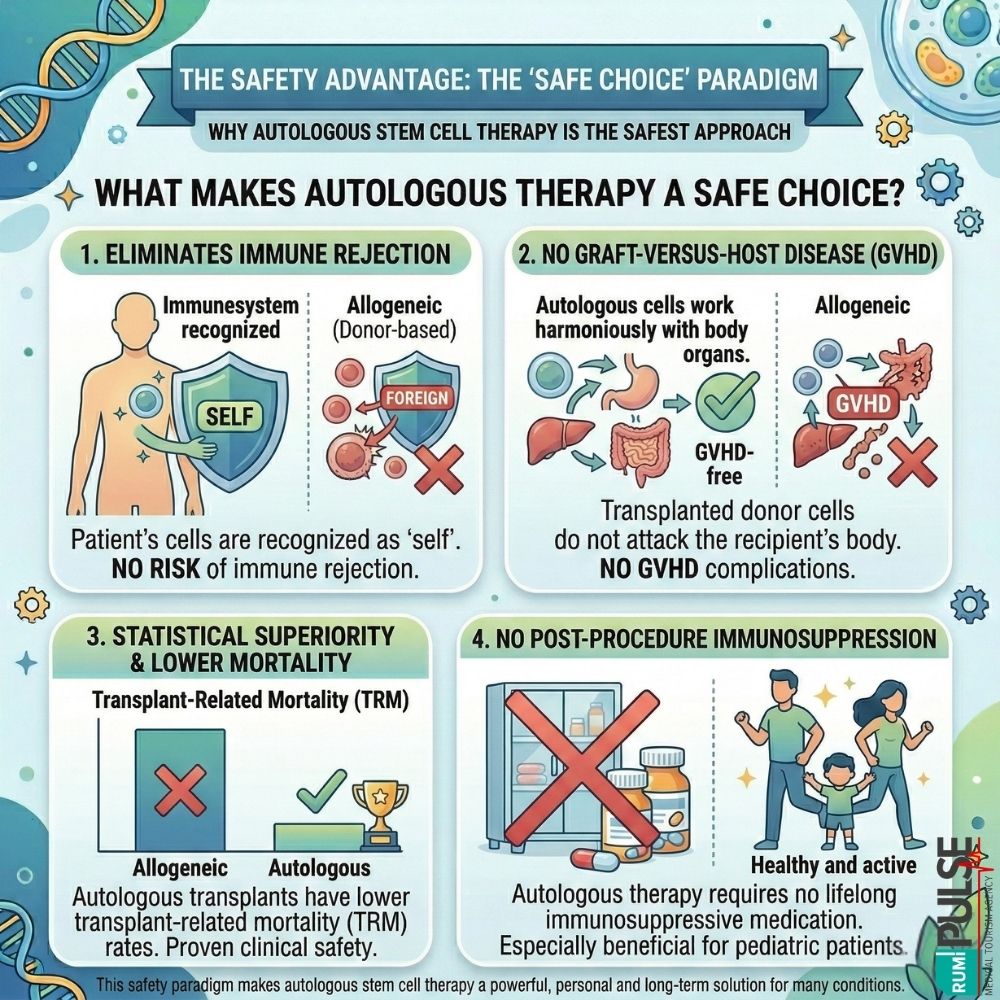
Safety is a major concern for patients considering biological therapy. Autologous stem cell therapy offers significant safety advantages over allogeneic (donor-based) therapies. Since the cells are the patient’s own, there is no risk of immune rejection or graft-versus-host disease (GVHD), a common complication in allogeneic transplants.
Key Safety Benefits:
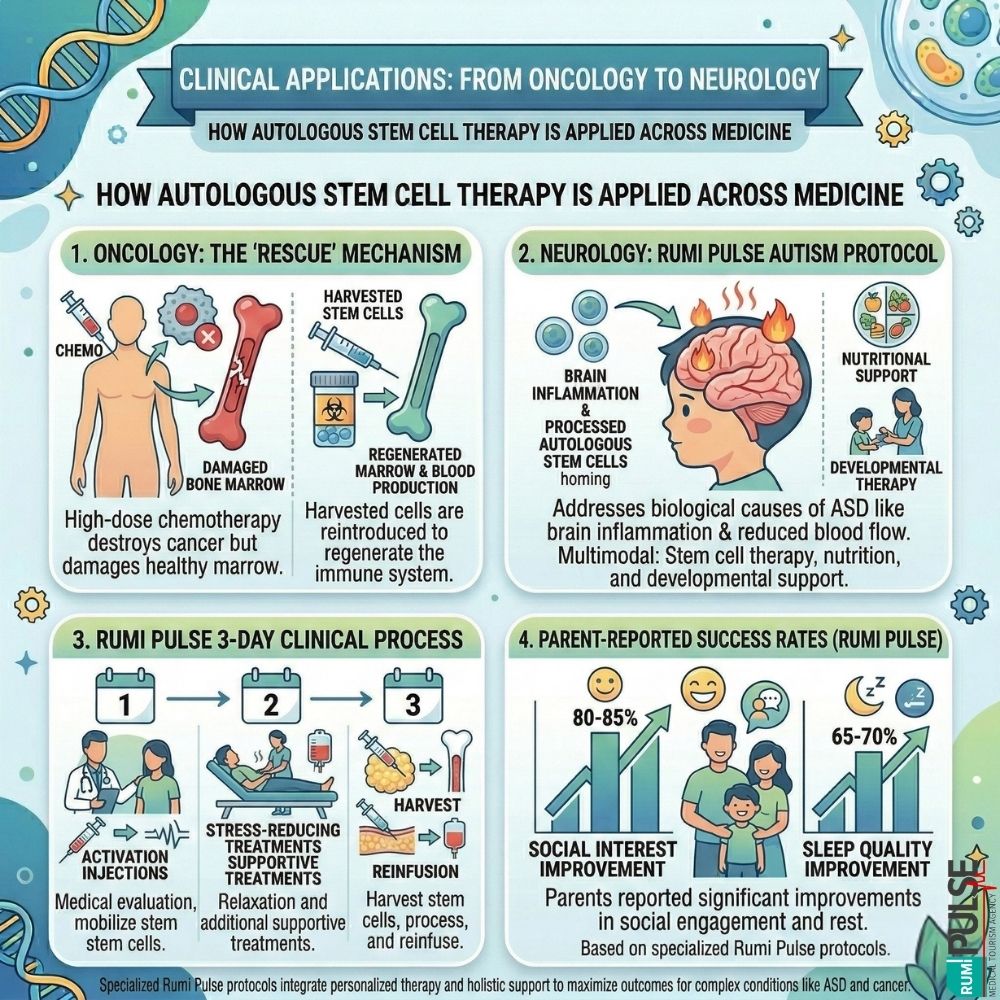
Autologous stem cell therapy has broad applications across various fields of medicine.
In blood cancers like multiple myeloma, autologous stem cell therapy is used to "rescue" patients after high-dose chemotherapy. Chemotherapy destroys cancer cells but also damages healthy bone marrow. By harvesting and freezing the patient’s stem cells before chemotherapy, these cells can be reintroduced afterward to regenerate the immune system and restore blood production.
One of the most innovative uses of autologous stem cell therapy is in the treatment of Autism Spectrum Disorder (ASD). Rumi Pulse has developed specialized protocols to address the biological causes of autism, such as brain inflammation and reduced blood flow. The Rumi Pulse approach combines autologous stem cell therapy with nutritional support and developmental therapy to optimize outcomes.
The 3-Day Clinical Process at Rumi Pulse:
Success Rates: Parent-reported outcomes show significant improvements in areas like social interest (80-85% improvement) and sleep quality (65-70% improvement).
The success of autologous stem cell therapy depends on a rigorous protocol:
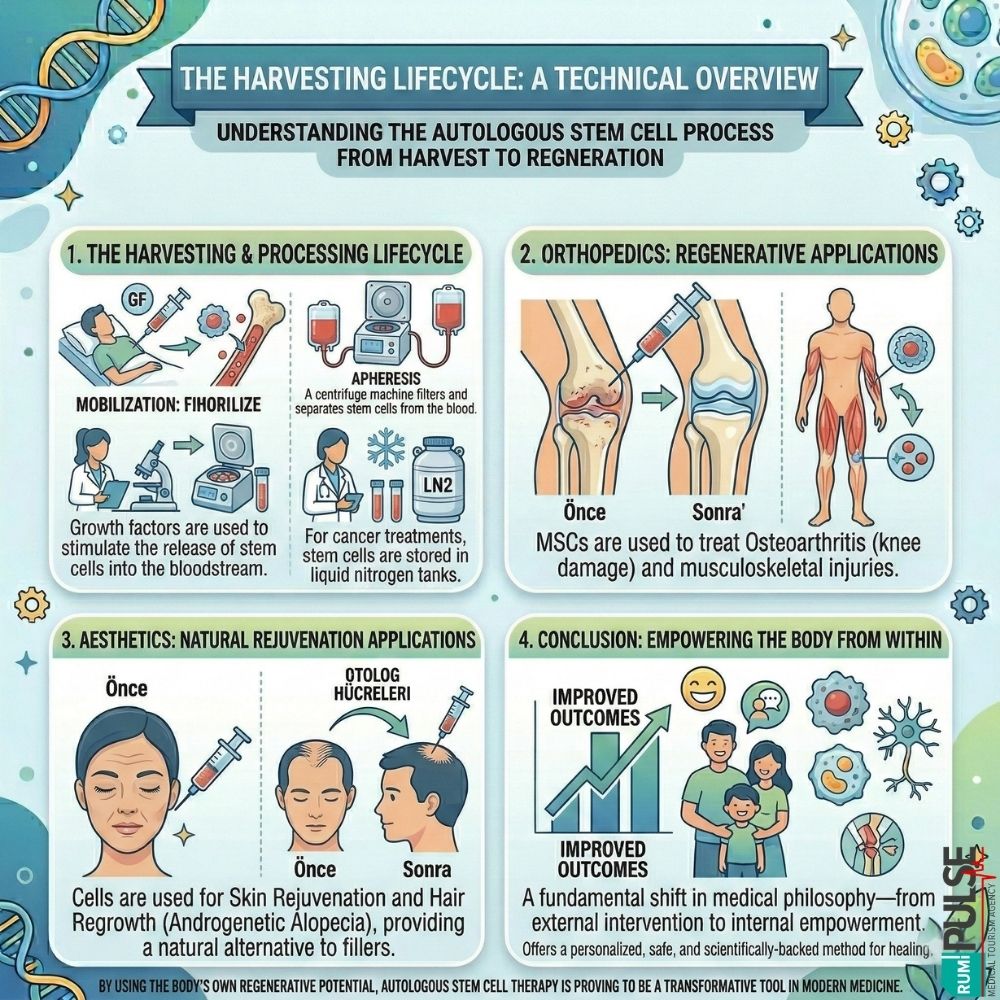
Autologous stem cell therapy is also making a significant impact in orthopedics and aesthetic medicine:
Autologous stem cell therapy represents a fundamental shift in medical philosophy—from external intervention to internal empowerment. By using the body’s own regenerative potential, this therapy offers a personalized, safe, and scientifically-backed method for healing. Whether for treating cancer, neurological disorders like autism, or musculoskeletal injuries, autologous stem cell therapy is proving to be a transformative tool in modern medicine.